Blog
Reveal Fresher, Healthier Skin with Acne Treatment Programs

Acne is one of the most common chronic inflammatory skin conditions worldwide, affecting adolescents and adults across different skin types. Although often perceived as a temporary cosmetic concern, acne represents a multifactorial medical disorder involving excess sebum production, follicular obstruction, microbial overgrowth, and immune-driven inflammation. When inadequately managed, acne can lead to long-term consequences such as scarring, persistent pigmentation, and psychosocial distress.
As people age, the biological behavior of acne often changes. Sebum production gradually declines after early adulthood, but inflammatory sensitivity may increase, epidermal turnover slows, and the skin barrier becomes more vulnerable to disruption. These shifts can make acne more persistent, more likely to leave marks, and more resistant to generic skincare approaches. For individuals exploring facial acne treatment Singapore, understanding how structured acne treatment programs support long-term skin health can help guide informed decisions about care.
Why Acne Management Matters Medically Over Time
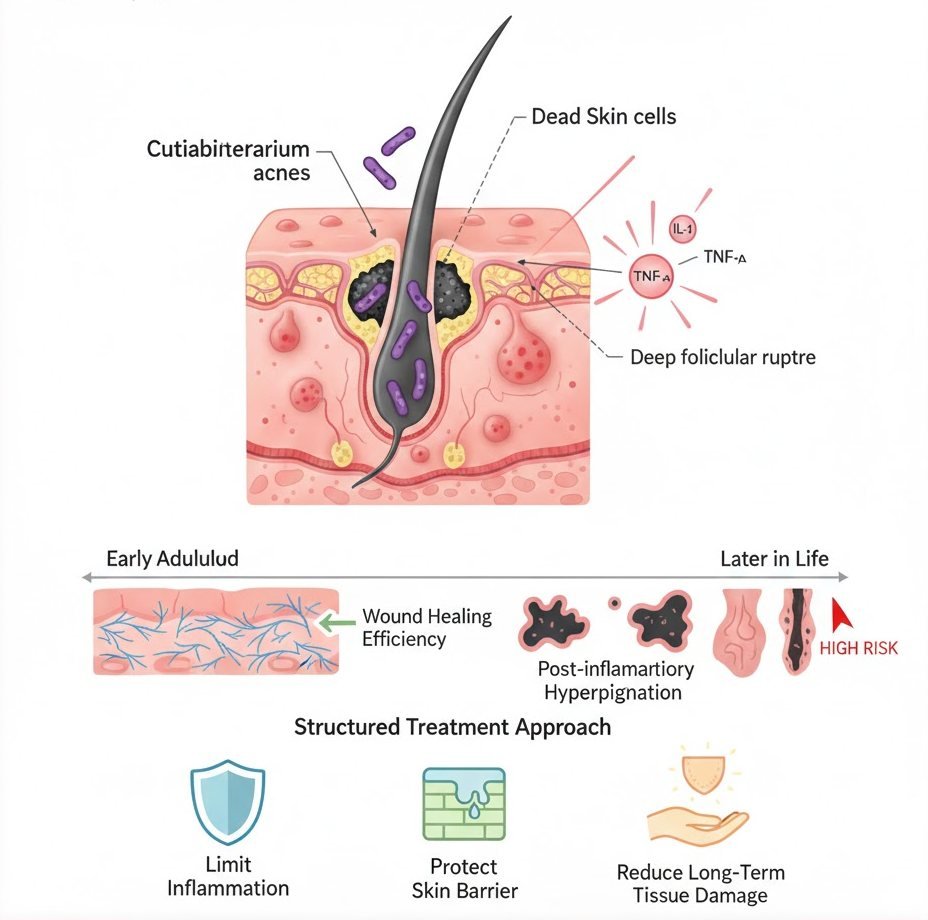
Acne develops within the pilosebaceous unit, where dead skin cells, oil, and bacteria accumulate within hair follicles. Cutibacterium acnes contributes to immune activation by stimulating inflammatory mediators such as interleukin-1 and tumor necrosis factor-alpha. This inflammatory cascade leads to redness, swelling, pustule formation, and, in severe cases, follicular rupture.
With age, the skin’s capacity to resolve inflammation becomes less efficient. Collagen production decreases by approximately 1% per year after early adulthood, wound healing slows, and post-inflammatory pigment changes persist longer. This means that acne flares later in life carry a higher risk of permanent scarring or discoloration than similar breakouts in younger skin.
A structured acne treatment approach aims not only to reduce visible lesions but also to limit inflammation, protect the skin barrier, and reduce long-term tissue damage.
Screening, Prevention, and Early Clinical Assessment
Early evaluation is a key component of effective acne management. Acne varies widely in severity, lesion type, distribution, and underlying triggers. Clinical assessment typically includes evaluation of:
- Comedonal, inflammatory, nodular, or cystic lesions
- Pattern of distribution (face, jawline, chest, back)
- Duration and recurrence of breakouts
- Presence of scarring or post-inflammatory hyperpigmentation
- Possible hormonal, medication-related, or lifestyle contributors
Early identification of patients at higher risk of scarring allows more proactive intervention. Nodulocystic acne, frequent inflammatory flares, and a family history of acne scars are factors that may justify more intensive management.
Screening also helps differentiate acne from acne-like conditions such as rosacea or folliculitis, which require different therapeutic strategies. A dermatologist may use this information to develop a treatment plan aimed at both immediate control and long-term prevention.
Daily Care and Lifestyle Factors That Influence Acne Outcomes
Daily habits strongly influence how acne responds to treatment. Over-cleansing, aggressive exfoliation, and harsh drying products can disrupt the skin barrier, increasing irritation and inflammatory signaling. Barrier disruption may paradoxically worsen acne by stimulating compensatory oil production and prolonging lesion healing.
Gentle cleansing with pH-balanced formulations is generally sufficient to remove debris without compromising barrier integrity. Non-comedogenic moisturizers containing ceramides, glycerin, or hyaluronic acid can help maintain hydration while supporting treatment tolerance.
Sun exposure also plays a role. Ultraviolet radiation can increase inflammation and prolong post-acne pigmentation. Broad-spectrum sunscreen with SPF 30 or higher is commonly recommended to protect healing skin and reduce contrast between affected and unaffected areas.
Lifestyle factors such as sleep quality, stress levels, and smoking may indirectly affect acne severity. Chronic stress elevates cortisol, which can stimulate sebaceous gland activity and inflammatory pathways. While lifestyle changes alone rarely resolve acne, they often influence how effectively medical treatments perform.
Age-Related and Chronic Conditions Linked to Acne
Acne in adulthood frequently overlaps with other chronic or age-related skin conditions. Hormonal acne, often seen along the jawline and chin, may be influenced by fluctuations in estrogen, progesterone, or androgens, particularly during perimenopause.
Rosacea may coexist with acneiform lesions, requiring careful differentiation because overly aggressive acne treatments can worsen facial flushing and sensitivity. Seborrheic dermatitis can contribute to scaling and irritation around the scalp and nasal folds, complicating acne management.
Individuals with eczema or sensitive skin may be more prone to barrier disruption and irritation, necessitating gentler treatment protocols. These overlapping conditions highlight the importance of individualized, medically guided care rather than uniform over-the-counter approaches.
Prescription Treatments Versus Over-the-Counter Options
Over-the-counter acne products often contain benzoyl peroxide at concentrations of 2.5–5% or salicylic acid at 0.5–2%. These agents may reduce bacterial load and promote exfoliation but frequently cause dryness or irritation if used excessively. They are typically most effective for mild or early acne.
Prescription treatments allow for more targeted and sustained modulation of acne pathways. Topical retinoids such as adapalene 0.1–0.3% or tretinoin 0.025–0.1% normalize follicular keratinization and reduce microcomedone formation. These medications often require 8–12 weeks of consistent use before visible improvement becomes noticeable.
Topical antibiotics, sometimes combined with benzoyl peroxide, help reduce inflammatory lesions but are generally prescribed for limited durations to reduce bacterial resistance. Oral antibiotics may be used for moderate to severe inflammatory acne, typically for defined treatment courses. Hormonal therapies and oral retinoids may be considered in specific clinical contexts.
Compared with over-the-counter products, prescription regimens generally offer higher efficacy for moderate to severe acne but require medical supervision to manage side effects and optimize long-term outcomes.
In-Clinic Procedures That Support Acne Treatment Programs
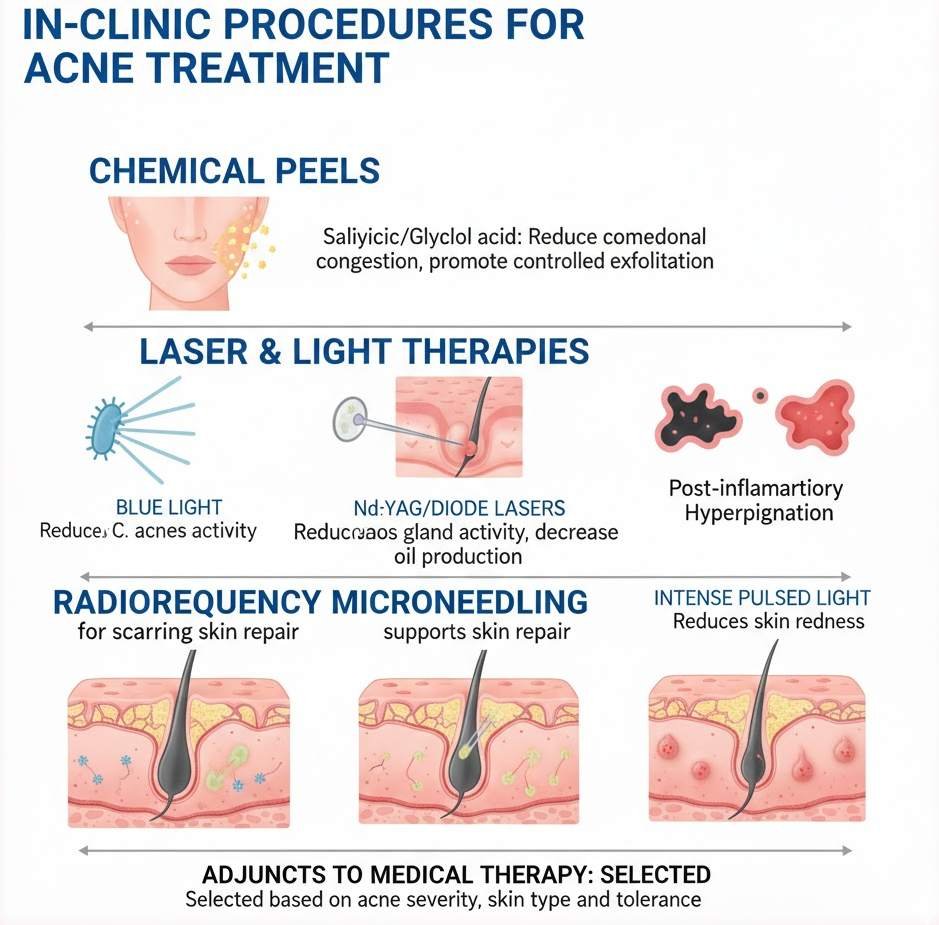
In-clinic procedures can complement medical therapy, particularly in patients with persistent inflammation, medication intolerance, or early scarring.
Chemical peels using low concentrations of salicylic or glycolic acid help reduce comedonal congestion and promote controlled exfoliation. These procedures are designed to improve lesion turnover without excessively disrupting the skin barrier.
Laser and light-based therapies target acne through different mechanisms. Blue light therapy reduces C. acnes activity by activating bacterial porphyrins. Nd:YAG and diode lasers deliver controlled thermal energy to reduce sebaceous gland activity, leading to gradual decreases in oil production.
Intense pulsed light (IPL) may reduce inflammatory redness and vascular signaling associated with acne. Radiofrequency microneedling is more commonly used for acne scarring but may also support dermal remodeling after inflammation is controlled.
These procedures are generally used as adjuncts rather than replacements for topical or systemic therapy and are selected based on acne severity, skin type, and patient tolerance.
What Our Aesthetic Clinic Says
In my clinical experience, acne outcomes are most stable when treatment is structured rather than reactive. Many patients arrive after trying multiple over-the-counter products, often alternating between overly harsh and ineffective regimens.
I focus on identifying the type of acne, understanding triggers, and building a sustainable program that balances efficacy with skin barrier preservation. Improvement usually occurs gradually over several months, and maintaining consistency tends to be more important than using the strongest possible product. Patients who view acne care as a long-term management process rather than a short-term fix often experience fewer relapses and better overall skin stability.
Putting This Into Practice
- Track how long acne persists and whether breakouts recur frequently
- Use gentle, non-comedogenic skincare rather than harsh drying products
- Apply prescribed treatments consistently and allow adequate time for response
- Protect skin from excessive sun exposure
- Attend follow-up visits to monitor progress and adjust treatment
When to Seek Professional Help
- Acne persists beyond adolescence or recurs frequently
- Breakouts are painful, cystic, or spreading
- Scars or dark marks begin to develop
- Over-the-counter products fail after several months
- Acne affects confidence, mood, or social interactions
- Adult-onset acne appears without a clear trigger
Commonly Asked Questions
| Question | Answer |
|---|---|
| How long should I try over-the-counter acne products before seeing a clinician? | If there is no meaningful improvement after 8–12 weeks of consistent use, professional evaluation is often reasonable. |
| Is adult acne different from teenage acne? | Yes. Adult acne is often more inflammatory, hormonally influenced, and slower to resolve, requiring tailored treatment strategies. |
| Do acne treatment programs always involve oral medication? | No. Many patients achieve good control with topical therapy and procedural support alone, depending on acne severity. |
| Can early treatment reduce the risk of acne scars? | Yes. Early control of inflammation lowers the risk of permanent scarring and prolonged pigmentation. |
| Will acne always require long-term management? | Not always. Some individuals experience remission, while others benefit from maintenance therapy to prevent recurrence based on underlying biology. |
Next Steps
Acne is a medical condition that often benefits from structured, evidence-based management rather than ongoing self-directed trial and error. If breakouts persist, recur, or begin to leave marks, a consultation with a dermatologist can help clarify underlying drivers and establish a treatment plan aimed at long-term skin stability and health.
